Automated re-credentialing is high impact: Work smarter, not harder


In the realm of a dental office, things are often moving fast: Patients are calling in to make appointments while others are checking in for appointments, and meanwhile, your team is presenting treatment plans, ensuring the patient experience is pleasant, and plowing through the billing process.
With so much happening in the day-to-day, re-credentialing each year or two is frequently an overlooked task at the dental office.
Traditionally, the re-credentialing process has been time-consuming and fraught with administrative challenges — and it must be completed accurately and on time, every time. Why so much urgency?
Because credentialing is required for dentists to be reimbursed by insurance providers for treatment of covered patients, and re-credentialing your dentists every year or two is necessary to maintain their status.
But re-credentialing happens so infrequently, it can feel like one of those tasks you set aside and will “get to,” despite its importance.
That’s why the advent of automated re-credentialing at DCS is revolutionizing the dental industry, offering significant time and cost savings while reducing administrative headaches and hassles.
Let’s dig into the many benefits — but first, why is re-credentialing so important?
Understand the importance of re-credentialing for dentists
First thing’s first: You must re-credential your dentists before the payer’s deadline. It’s crucial for your billing and compliance. This isn’t a task you can avoid or put off — though you can delegate it to a service provider.
Insurance companies need to confirm that the dental practitioners in their network are still professionally qualified. Re-credentialing is the process insurance companies use to verify those qualifications, specifically:
- The dentist’s license is in good standing
- The dentist is qualified according to the insurer’s current eligibility criteria, and
- The dentist’s information is up-to-date.
Insurance companies will typically mail a dentist a reminder when it’s time to be re-credentialed — but don’t wait to send in the required documents. You must submit them right away to get the process started, or risk an interrupted cash flow and unhappy patients.
Related: 3 ways dental credentialing issues can cost your practice
According to the ADA:
“Dentists have reported waiting up to 6 months to get credentialed with certain commercial and state insurance plans. This can be disruptive to patients who are waiting for doctors to get credentialed so that they can receive the benefits of seeing a network provider.”
The good news is that you no longer need to dread the re-credentialing process. Now it can be automated, and you can trust that it’s taken care of on time, every time, with little to no effort on your part.
Now, let’s explore the 3 top benefits to automating your re-credentialing process…
Benefit #1: Automated re-credentialing saves time
Automated re-credentialing streamlines the entire process, eliminating the time your team spent on paperwork and follow-ups. This efficiency translates into improved workflows, allowing dental staff to focus more on patient care and less on administrative tasks.
The traditional dental credentialing process can take six months or more. If you pass your application deadline while you play the waiting game, you won’t be able to bill insurance companies for your services. This leads to strained finances and, ultimately, the inability to deliver high-quality patient care.
Fortunately, now there’s a better way — and it's more user-friendly because you can finally see how far along your application is in the process.
Instead of your team and your patients — and your revenue — possibly being held back by the months-long wait for a dentist to be re-credentialed, automate this process and have it managed efficiently.
Automated credentialing and re-credentialing services are available at DCS via a subscription service.
With your subscription to DCS Credentialing, you’ll have access to an up-to-the-moment view of your credentialing status on a clean, easy-to-use dashboard that’s available 24/7.
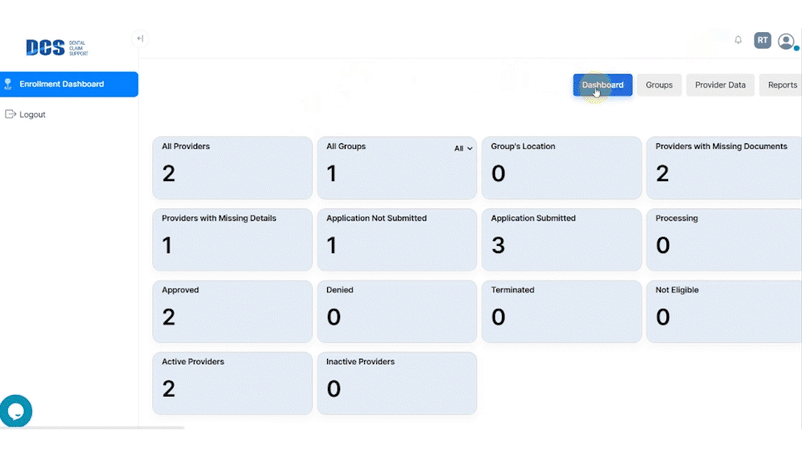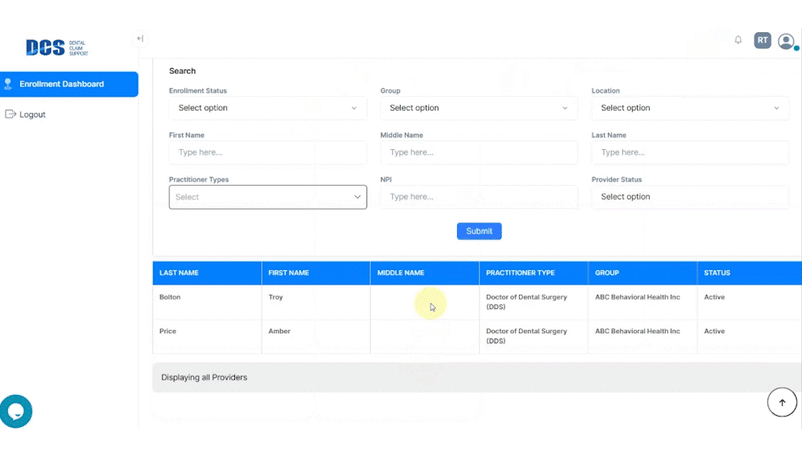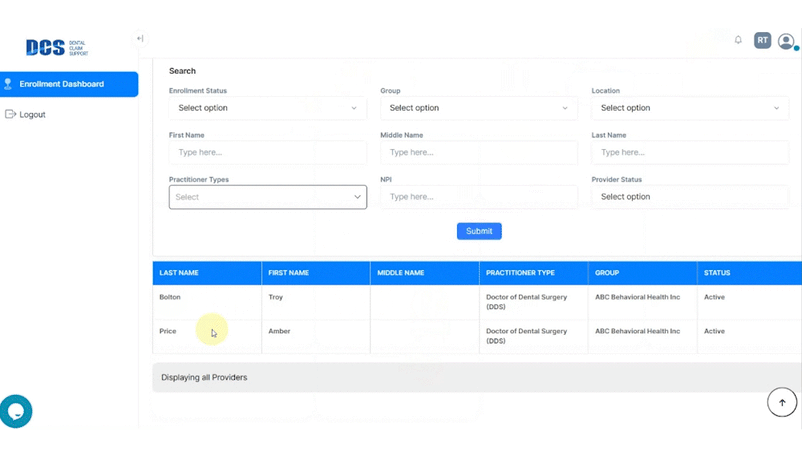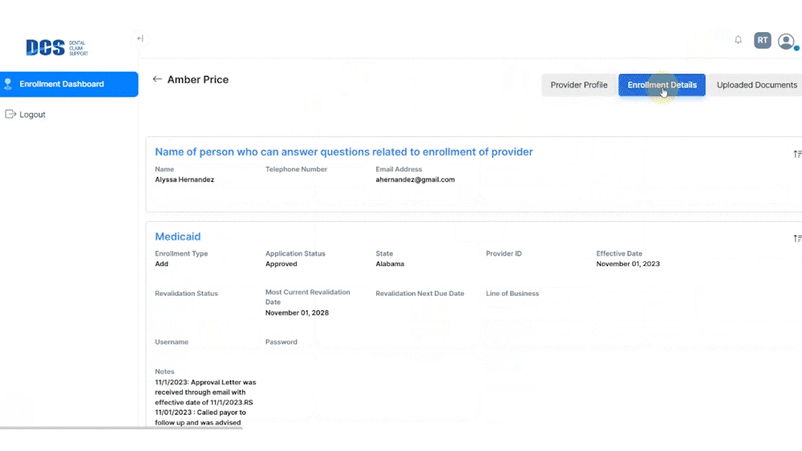
In the meantime, your team can use their valuable time to focus on running your dental business and taking care of your patients.
Benefit #2: Automated re-credentialing saves money
Efficient credentialing delivers faster cash flow, because you can continue billing and receiving payments for services for consistent revenue. Missing the deadline results in a lull in providing covered services while you wait weeks, or even months, for status approval.
During this lull, you aren’t in-network with big insurance companies, and you might have to turn away patients or require them to pay out of pocket, or you’ll risk not getting reimbursed from insurance as in-network.
If your credentials are not up-to-date, and you’re listed as the providing doctor on a claim, that will surely result in an immediate claim denial.
DCS’ Assistant VP of Strategy and Special Projects, Will Snipes, explains DCS credentialing services, specifically:
"In our system there is a transparent view as to when the re-credentialing dates roll around for the provider to see themselves, that our team also monitors. We seamlessly and proactively begin the re-credentialing process on their behalf and make sure that all documents are current.
The idea behind it is that we work to initiate that process with the provider office before they notify us they need to be re-credentialed.”
Related: Top 5 mistakes dentists make in the dental credentialing process
A service gap in the re-credentialing interval means your practice or group misses out on revenue and opportunities to grow your practice. But when you automate your credentialing and re-credentialing process, you won’t lose money — in fact, you’ll save money.
These savings come not just from reduced administrative expenses, such as mailing, postage, and time; but also from avoiding delays in insurance processing and reimbursements that we mentioned before.
Benefit #3: Automated re-credentialing eliminates administrative headaches
One of the biggest challenges in traditional re-credentialing is the administrative burden it places on your in-house staff. But when you automate your re-credentialing, your team’s administrative burden disappears.
Specifically, our automated credentialing services at DCS take care of:
- Payer enrollment, facility enrollment, and re-enrollment
- Quarterly provider enrollment service maintenance
- As-required services, including:
- Screening for network/enrollment paneling with payers, including those relative to the practice
- New provider setup services
- Monthly provider monitoring for sanctions and exclusions under the practice Tax Identification Number (TIN) and/or National Provider Identifier Group Number
- NPI 2 Enrollment
- 50-state inclusive background verification services
Imagine your team’s sighs of relief when they realize they no longer have to manage — or even think about — anything on that list.
Related: 3 common dental re-credentialing questions answered
With technology-based credentialing, you’ll minimize submission paperwork and follow-up tasks for your team, which then frees them to focus on patient care and enhance the overall efficiency of your dental business.
And the bonus for you: You’ll never again be left in the dark about your credentialing status.
Don’t wait to become re-credentialed: Start automating your process TODAY
To recap, here are 3 major benefits to automating your credentialing and re-credentialing process:
- Benefit #1: Automated re-credentialing saves time
- Benefit #2: Automated re-credentialing saves money
- Benefit #3: Automated re-credentialing eliminates administrative headaches
The subscription-based DCS Credentialing service promises a high-speed and efficient dental credentialing process that streamlines operations to boost revenue, ensure compliance, and maintain consistent cash flow.
Let us simplify credentialing for you: Book a call today.
Related Posts
Dental revenue resources from Dental Claim Support


