You just outsourced your dental insurance billing, now what? 5 things you’re still responsible for
.jpg)

You’ve just outsourced your dental insurance billing and now you’re thinking, “what do I do now?” You’re working with a company that’s supposed to take over the insurance billing that used to take up hours in your administrative team’s day, and now you’re wondering what’s next.
At Dental ClaimSupport, we have built our business on processes and relationships. We have seen many practices thrive by embracing working with a dental billing company. One thing we have noticed with those practices that don’t get the most from their remote support: a failure to understand in-house responsibilities.
When outsourcing, creating a good working relationship between your remote dental billing team and your office staff is essential to the success of the process within your office.
Most people think if you outsource your dental billing, that you have to eliminate an employee in your office. This couldn’t be further from the truth. In fact, you’ll see there are plenty of daily tasks to be performed at the front desk that you can better attend to now that someone else is dealing with insurance companies.
This article will clarify the responsibilities your staff will still need to be focused on to make your practice profitable and successful while creating a healthy working relationship with the dental billing company.
Here are 5 things your in-house staff should continue doing for your practice to be successful:
1. Verifying dental insurance
This step in the dental billing process is arguably the most important because it sets the stage for how the rest of the dominoes fall. Insurance verification means your office is checking a patient’s insurance coverage and benefits before the date of service to ensure eligibility and future payment for services.
This process confirms not only that the patient has active dental coverage, but also what procedures are covered by their dental insurance.
This is such an important step because you can figure out how much of the cost the patient will be responsible for prior to the procedure, and you can communicate that with confidence. You can also communicate any fine print they should be aware of such as:
- Frequency limitations
- Waiting periods
- Missing tooth clauses
- Replacement clauses
Talking about money and insurance is sensitive, which is why it is better for the in-house dental office team to do so. You are a familiar face and most patients would prefer you talk in person with them instead of a stranger over the phone.
2. Patient AR (Accounts Receivables)
Your office will handle all patient billing and AR. There are a few key responsibilities here to remember such as collecting patients’ co-pays, sending patient statements, and going through your patient aging report to call them about any outstanding payments.
You will collect dental patient co-pays
As you know, a co-pay is the fixed amount for a covered service, paid by a patient to the provider of service (your office) before receiving the service. Collecting co-pays in the office face-to-face is a much better experience for your patients, and more likely to keep your patients happy and willing to cooperate than if a remote billing service called them for payment.
As mentioned before, money can be sensitive. Asking for a co-pay is pretty straightforward, and this is the rare information that most patients are aware of when it comes to their insurance (because it usually says it right on their card!) Still, wouldn’t you rather pay someone in-person that you know rather than a stranger over the phone?
You will send monthly patient statements
Your staff will be responsible for sending dental patients their statements. Whether this means mailing them or handing a copy of it to them right after their procedure, it is your responsibility to make sure your patient has a breakdown of what procedures cost, how much their insurance covers, and what their out-of-pocket balance is.
Patients appreciate having clear information for their own record-keeping. Each statement you prepare and send documents that you have clearly communicated what procedures have been performed, what it cost, and how their insurance benefits have been applied.
This way there is no confusion for either your office or the patient.
3. Contacting your patients
Sometimes information changes, or was entered incorrectly to begin with. These changes could include a new insurance policy or address change. Incorrect information could also be a result of data entry errors. It happens, we’re all human here. However, you want to make sure it gets updated ASAP. Time to pick up the phone and call the patient.
This goes right back to you knowing your patient better than anyone. If you got a call from a stranger you’ve never met asking about personal information such as your insurance, wouldn’t you immediately suspect it’s a spam call? Sure, they aren’t asking about your car’s “extended warranty” but you don’t want your patient thinking it still sounds spammy.
When the patient gets a call from a number they recognize and a name they remember, they will happily give you any update to their personal or insurance information.
Want to avoid losing patients because of insurance? Read about how billing mistakes will make them leave your practice and how to avoid these missteps.
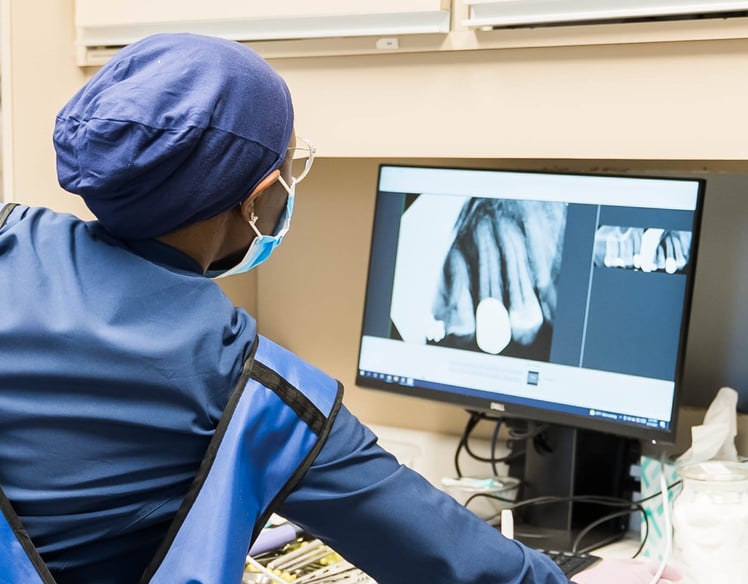
4. Handling x-rays & clinical notes
Your office will still need to write clinical notes in your patient charts explaining why a procedure was performed. It’s important that you handle notes and narratives in the office so that you can easily ask the dentist any questions about a procedure.
Your clinical team will take the proper x-rays. You saw the patient, did the work, and you know why the service was performed.
All of this should still be documented by the in-house clinical team in the chart notes and clinical notes. Documenting any patient visit, why procedures were performed and/or diagnosed, will always be a responsibility of the doctor, assistant, or hygienist.
.jpg?width=731&name=DSC05809%20(2).jpg)
Overlooking the need for necessary x-rays and clinical notes is a surefire way to have insurance companies deny a dental claim.
Having proper x-rays and clinical notes easily accessible will eliminate extra work on your staff when submitting dental claims AND appeals.
The billing company will, in turn, take this documentation and use it to send claims accurately with attachments. These notes will also be used to dispute rejected claims and send appeals.
5. Creating and Batching Claims (Not Sending)
The dental billing company will send the claims and do the leg work with following up on the claims, but you have to create and batch them. Here’s why: the dental billing is working remotely. They do not know if patients from the schedule were present or not.
The dentist is ultimately responsible for any and all claims that are submitted from the practice. It’s essential that patients are walked out and claims are batched by an in-house staff member.
The software is set to indicate whether that code is going to be submitted to the insurance company or not. It’s pretty easy! And you can do it right after the patient leaves the dental office or even as they’re checking out. The dental billing company will take it from there to make sure your claims get paid by insurance.
When it comes to sending the batched claims through your clearinghouse, which includes adding attachments and narratives, your outsourced dental billing will likely handle this task for you.
Let a dental billing company take care of the background work at your dental practice
Hiring a dental billing company means you no longer have to wait on the phone following up on outstanding claims, spend hours working on your insurance aging report or follow up on claims that you barely remember creating in the first place.
Once you have the claim support from a dental billing company, you can focus on what’s in front of you in the office, such as insurance verification, making sure patient information is correct, collecting from patients, and creating claims.
This will ensure your patient has the best experience possible at your practice, and you don’t have to worry about communicating with insurance companies.
Now that you’re aware of your responsibilities when you hire a dental billing company, learn how to cultivate the best relationship with your remote dental billers in our Learning Center.
Related Posts
Dental revenue resources from Dental Claim Support

